
'I spent a whole year indoors and upstairs.' Life during the pandemic for people with disabilities
This was not out of choice. It was not as if the 73-year-old wanted to be there, forgoing having the sun on his face, and enjoying the views of the small lake at the bottom of his garden in a town on the outskirts of Glasgow, Scotland. It was because his stairlift broke in late March 2020, days before the UK went into a nationwide lockdown.
Elder-Woodward, a former social work officer from Glasgow City Council, was born with cerebral palsy and requires round-the-clock care as he cannot walk and uses a wheelchair. The stairlift has been a provision for 30 years, he said, yet his local authority -- the West Dunbartonshire Council -- refused to pay for a replacement, saying his "bed could be moved downstairs to the living room," Edward-Woodward told CNN. "But my bathroom and my study are upstairs," he added.
In order to consider granting him a new lift, the council had to make an assessment of his needs, but this could only be done after lockdown, Elder-Woodward said.
Council officials eventually visited in late spring and agreed in June to cover some of the costs of his new lift, he said, as the old one was condemned as unfit. But the installation of a new lift in his 19th century house required architectural and structural drawings, and building control approval, which can take months. Along with further delays fueled by the pandemic such as restrictions, working from home and social distancing, this meant construction only began last week.
"Throughout the pandemic, the HSCP [health and social care partnerships] have had to prioritize care to those most at risk," a spokesperson for West Dunbartonshire Council told CNN. "We have kept in close contact with Mr Elder-Woodward throughout this period and are pleased that the installation works have now been able to commence."
But for the past year, Elder-Woodward has been unable to hold his fiancée, who also uses a wheelchair. "She lives in her own flat and when she comes here, they communicate by talking up the stairwell," Jeanette Young, one of his carers, told CNN. Carrying him up and down the stairs is not an option because he is "bloody heavy," she added with a throaty laugh.
'An afterthought at best'
Elder-Woodward's ordeal is just one of the many problems people with disabilities have had to endure during the pandemic and experts say this is unsurprising to them.
"The lack of preparedness for the impact of the pandemic on disabled people has been shockingly familiar," write disability experts, including Thomas Shakespeare, a professor of disability research at the London School of Hygiene and Tropical Medicine (LSHTM), in a commentary published in the Lancet earlier this month.
"Ignored at worst, and an afterthought at best," people with disabilities have experienced a three-fold risk during the outbreak, the authors argue: a bigger risk of severe or fatal outcomes from the disease; greater risk of reduced access to routine healthcare and rehabilitation, even though disabled people on average have a narrow margin of health; and harmful social impacts of efforts to mitigate the pandemic, they write.
They also highlight a World Health Organization report that identified people with disabilities as typically being more likely to be older, poorer, experience co-morbidities, and be female -- of which three factors are linked to a greater risk of severe Covid-19 disease or death.
According to the UK's Office for National Statistics (ONS) the risk of death involving Covid-19 in England between January 24 and November 30, 2020 was up to 3.1 times greater for disabled men, and up to 3.5 times greater for disabled women, than for non-disabled men and women.
The ONS analysis also showed that in the first wave of the pandemic, between March and November 2020, people with disabilities made up almost 60% of all the deaths involving Covid-19 despite only accounting for 17.2% of the population in England.
There are reasons to suspect that people with disabilities will be more likely to die in the pandemic, said Hannah Kuper, co-director of the International Centre for Evidence in Disability at the London School of Hygiene and Tropical Medicine "They are more likely to live in deprivation, be older, overweight and live with carers or in care homes where it is difficult to socially distance," she explained.
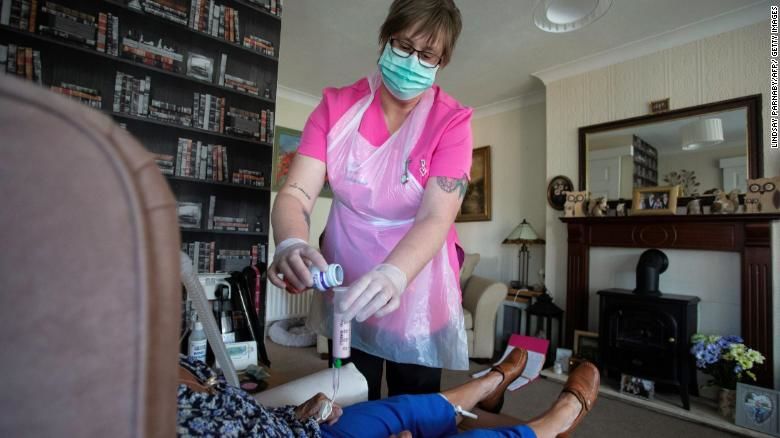 Many people with disabilities live in care homes and rely on carers.
Many people with disabilities live in care homes and rely on carers.
A November report by Public Health England found that the virus accounted for more than half of all deaths of adults with learning disabilities in care homes between April and May 2020. But it took almost a year for this impact from the pandemic to be recognized.
The UK's vaccination campaign began in December and targeted four priority groups to begin with, including people over 70 and anyone who is clinically extremely vulnerable. But it was only in February when the Joint Committee on Vaccination and Immunisation (JCVI) expanded its priority groups to include people with learning disabilities. This was following the release of a study that found that people with learning disabilities were up to five times more likely to be hospitalized with the disease and up to eight times more likely to die compared to the general population, according to Kuper, who led the research.
The issue is compounded by various failures during the pandemic. For example, late last year, the regulator for England's health and social care services, the Care Quality Commission (CQC), found that "Do Not Attempt Cardio-Pulmonary Resuscitation" notices (DNACPRs) were wrongly placed on some care home residents with learning disabilities at the start of the pandemic, potentially causing avoidable deaths.
The notices are placed on people too frail to receive CPR, but learning disability charity Mencap said that fit and healthy people with learning disabilities may have had DNACPRs placed on them. In a follow up report, released Thursday, the CQC found that more than 500 people were put on "do not resuscitate" orders without their consent or their carers' consent.
But for people with disabilities who have managed to avoid catching the coronavirus this past year, like Elder-Woodward, the pandemic has brought other struggles, highlighted in a study released last month as a pre-print by Shakespeare and his team at the LSHTM.
'Impact beyond the risk of getting ill and dying'
The researchers explored the lived experiences of people with disabilities during the first wave of the pandemic in the UK. During interviews, people who were blind talked about the increased stigma they faced because their impairment meant they had trouble maintaining social distance. "Guide dogs don't understand social distancing," Shakespeare told CNN, adding that a blind person he interviewed was shouted at when their dog cut the queue and went straight into the post office.
Blind people also spoke about the challenges of living without physical contact, like touches and hugs. "As a blind person I'm missing out on the whole lot because of social distancing," a participant said in the study.
People who were deaf or hard of hearing talked about face masks making it harder for them to understand what others were saying. Those who depended on food deliveries suddenly found themselves battling with the tens of thousands of non-disabled people avoiding the shops and doing an online food order.
Pandemic restrictions also saw the shuttering of large sections of the social care system, leading to people with disabilities being increasingly reliant on their family and other informal carers, the report notes. Facilities and events, such as day centers, art projects, or drama projects also got canceled or put on hold and Elder-Woodward, who was also a participant, said the only additional support offered in the pandemic by his local authority was a 15-minute home care visit to make him comfortable in his wheelchair.
"The impact of that is they then don't have any contact with other people... so the impact of that is they are watching television all day," Shakespeare said.
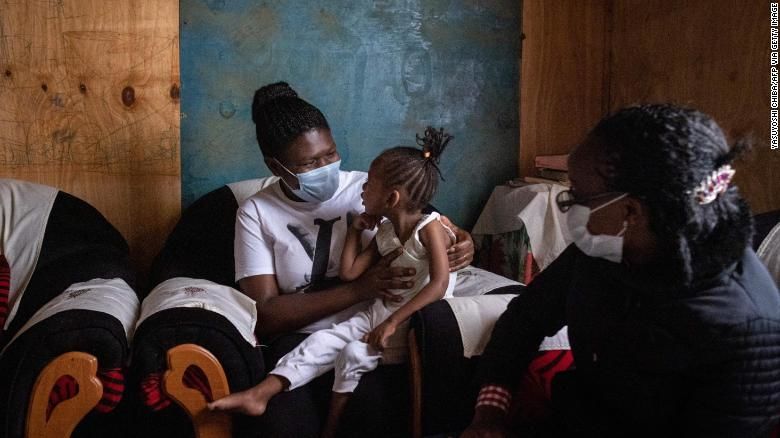 A consortium of international disability rights groups have urged
national governments to ensure persons with disabilities are recognized
as a priority group in vaccination plans.
A consortium of international disability rights groups have urged
national governments to ensure persons with disabilities are recognized
as a priority group in vaccination plans.
Parents and guardians of young people spoke of how their disabled children lost up to a year of therapy education and socialization. "Children with cerebral palsy need speech language therapy, they need physiotherapy or they lose their critical windows [to develop]," Shakespeare said, adding that older adults diagnosed with dementia, who have been sequestered away due to pandemic restrictions, are losing skills and suffering from increased memory loss.
"This all shows how the pandemic has an impact beyond the simple risk of getting ill and dying," he said. "There are lots of other ways in which disabled people, because they are more vulnerable or more at risk, are affected by the pandemic."
'Overwhelming' failure on a global level
A global report by human rights group the International Disability Alliance, which included respondents from 134 countries, found that policymakers "have overwhelmingly failed to take sufficient measures to protect the rights of persons with disabilities in their responses to the pandemic."
People surveyed said emergency health care was denied to adults and older persons in institutional settings, while others said they were abandoned by their governments and trapped at home with no means to access food, medicine or other basic supplies.
Uganda, Nigeria, Kenya, Bangladesh, India, Tanzania and Peru were among the countries with the highest percentage of respondents reporting no access to food. But this also occurred in several high-income nations, with more than 25% of respondents in the US, Canada, France and Belgium saying they struggled to access a meal. In some African countries people spoke of being harassed or beaten up by officials for breaking curfew or restrictions as they attempted to find food, the report writes.
In the US, a group of specialists argued in a letter to the American Journal of Psychiatry in August that the pandemic disproportionately affected people with intellectual and developmental disabilities -- many of whom lost the critical support they need but have been unable to advocate for themselves.
According to Kuper, the only available evidence that she has been able to find on how Covid-19 has disproportionately affected disabled people comes from the UK. Citing ONS data, a consortium of international disability rights groups called on United Nations agencies and national governments this March to ensure persons with disabilities are recognized as a priority group in vaccination plans.
Close to freedom
Not being able to go outside for a year means Elder-Woodward had a lot of time to fill. He has done so by studying for a part-time masters degree in philosophy at Glasgow Caledonian University, which he describes as a "hobby to keep my brain active." The internet has kept him company, and as the chair of a number of disability charities, attending a Zoom meeting is a daily occurrence.
While busy, he must also remain responsible for his own social care. He pays a team of five part-time personal assistants up £8,000 with the help of funding from the local authority, the government and his savings. They are a vital part of his life, running the day-to-day chores Elder-Woodward is unable to do from a wheelchair, including bringing food up from the downstairs kitchen.
But two of his assistants had to self-isolate as the first lockdown progressed, and another resigned, leaving only two carers available to cover the whole week. This meant he had six-hour periods without help, or company, and once found himself in the uncomfortable position of "being sat on my testicles" for hours as he was not able to readjust his body after a bathroom break.
"My life is completely different. I used to go out for meals, the cinema, go to the theater and see plays," Elder-Woodward told CNN. "Now all I can do is move between my bed and the study." He admits he is luckier than most, having 24-hour cover, but said it had been a constant battle to be able to preserve his autonomy. "Everything is a fight," he said. "They don't give you things willy-nilly."
Last Sunday, the installation of his lift was completed and Elder-Woodward was finally wheeled out to freedom. His first stop? "I had dinner with my fiancée," he says.











